Vancomycin Dosing Guidelines: What You Need to Know
In this article:
The 2020 vancomycin dosing guidelines from four leading pharmacy and infectious diseases professional societies – ASHP, IDSA, PIDS, and SIDP – were published in advance online in the American Journal of Health-System Pharmacy.
The 2020 vancomycin dosing guidelines represent a major paradigm shift in how hospitals, physicians, and home infusion services providers will be managing intravenous vancomycin dosing moving forward.
One of the biggest changes from the last vancomycin dosing guideline published in 2009 is that experts recommend moving from dosing based on trough to dosing based on area under the curve (AUC) for adults and pediatrics who have suspected or definitive serious MRSA infections.
By definition, serious MRSA infections include infections such as bacteremia, sepsis, infective endocarditis, pneumonia, osteomyelitis, and meningitis.
Vancomycin Dosing: What’s Changed?
From Vancomycin Trough Levels To Area Under The Curve
Over the last several decades, the guidelines for intravenous vancomycin dosing and monitoring have slowly shifted.
For years, pharmacists and clinicians would obtain both a peak and a trough to assess therapy. Then in the 2009 vancomycin dosing guidelines, the evidence available at the time indicated that the inclusion of peaks as part of the monitoring did not reduce vancomycin-induced nephrotoxicity and therefore, they were no longer recommended.
Now, based on clinical evidence that has evolved over the past several years, the recommendation to monitor vancomycin based on serum trough levels alone has been removed from the 2020 vancomycin dosing guidelines.
The guideline experts are now recommending dosing vancomycin based on an Area Under the Curve (AUC) and have established the relationship between vancomycin dosing to AUC and the minimum inhibitory concentration (MIC) or AUC:MIC as a “useful pharmacodynamic parameter to predict effectiveness.”
Patients dosed via a targeted AUC have shown to have a lower incidence of acute kidney injury.
The new 2020 vancomycin guidelines promote the following pharmacodynamic targets:
- For adults and pediatrics, the desired target AUC:MIC ratio is 400-600.
- In neonates targeting a minimum AUC:MIC of 400 is desired.
For both of these targets, the empiric MIC is generally assumed to be 1 mg/L based on broth microdilution (BMD). This is based on national vancomycin susceptibility surveillance data.
Breaking Down Vancomycin AUC:MIC
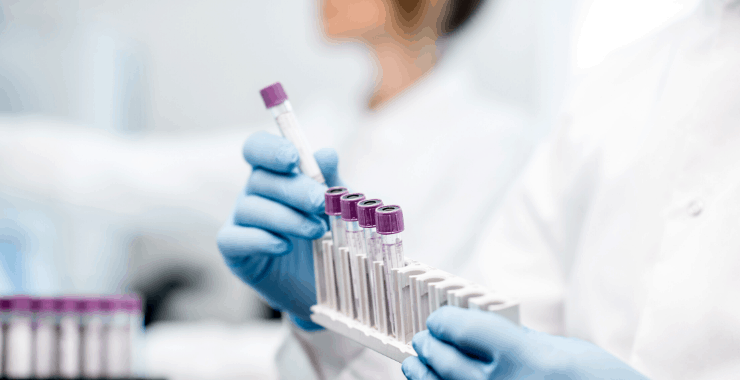
Vancomycin Area Under The Curve (AUC)
If we look at AUC:MIC, there are two parts, and both are addressed by the vancomycin dosing guidelines.
AUC vancomycin dosing represents the total vancomycin concentration in the blood over a period of time, usually over 24 hours.
In order to calculate this manually:
- Two vancomycin levels need to be drawn when the patient’s vancomycin is at a stable concentration, usually referred to as steady-state.
- Usually, the first level is drawn 1-2 hours after the vancomycin infusion is complete (referred to as a vancomycin peak) and the vancomycin trough is drawn at the end of the dosing interval (or restated, prior to the next dose of vancomycin).
- Then, using a series of complex calculations, vancomycin AUC can be calculated.
Vancomycin Minimum Inhibitory Concentration (MIC)
The other component to this key target pharmacokinetic/pharmacodynamic metric is the MIC. The reference method or “gold standard” for calculating MIC is called broth microdilution (BMD).
Although this is a highly accurate measurement of MIC, this is not easily replicated in the clinical setting.
Most clinical laboratories utilized automated methods of calculating MICs, but these are known to have discrepancies in the values reported when compared to BMD.
However, despite these differences, MICs are still generally treated the same in the lens of the vancomycin dosing guidelines.
Since national surveillance data shows that in most cases the MICBMD can be assumed to be 1 mg/L or less, this is generally the default value that is used in the absence of MICBMD information.
Interestingly, the vancomycin dosing guidelines state that even if the MICBMD is less than 1mg/L (e.g. 0.5 mg/L), the authors do not recommend decreasing the dose to achieve the AUC/MIC target.
In the case where the MICBMD is more than 1mg/L, there is a low probability of achieving and AUC/MIC target of 400 or above with conventional vancomycin dosing. In these cases, non-vancomycin therapy may be considered.

Vancomycin Dosing and Monitoring: What’s the Preferred Approach?
Based on the vancomycin dosing guidelines, the preferred approach to monitoring vancomycin dosing to AUC is through the use of Bayesian dosing software programs, such as DoseMeRx.
Why Bayesian Dosing for Vancomycin Dosing?
Pharmacokinetic models that have richly sampled vancomycin data (referred to as the Bayesian prior) inform the science behind Bayesian dosing software.
While two levels are still preferred according to the 2020 vancomycin dosing guidelines, when using Bayesian dosing an AUC can be calculated with just a single vancomycin trough level in select patients.
Other advantages to Bayesian dosing include:
- Levels can be obtained within the first 24-48 hours of therapy, meaning you do not have to wait until steady-state in order to obtain vancomycin concentration levels.
- Bayesian models are dynamic – the individualized PK/PD model is continuously learning over time and can be used to generate a dose recommendation at any time, not just when you have levels.
- Bayesian AUC guided vancomycin dosing can be applied to both pediatric and adult populations.
Vancomcyin Loading Dose: To Load or Not to Load?
Vancomycin Loading Dose
The vancomycin dosing guidelines are comprehensive in providing dosing recommendations for all age categories – neonates, pediatrics, and adults.
However, loading doses are not necessary for all patients but may be helpful in rapidly achieving therapeutic vancomycin blood levels in patients who are critically ill.
Adult and Obese Populations: What the Guidelines Recommend
The 2020 vancomycin dosing guidelines offer some clear guidance regarding loading doses and maximum doses:
- For non-obese adult patients with normal renal function, a loading dose of 20-35mg/kg (maximum dose: 3000mg) is recommended.
- For obese patients, a loading dose of 20-25mg/kg using actual body weight, up to a maximum dose of 3000mg may be considered.
- For empiric maintenance doses in non-obese, the guidelines recommend vancomycin 15 to 20mg/kg based on actual body weight administered every 8 to 12 hours. When the patient is obese, they recommend calculating the initial dose using population pharmacokinetics and that empiric maintenance dose do not exceed 4500mg/day (depending on renal function).
Pediatric Populations
In pediatric patients, there is insufficient data to base a loading dose recommendation in normal-weight patients. Interestingly, the vancomycin dosing guidelines state that in obese pediatric patients, a loading dose of 20mg/kg may be considered (assuming normal renal function).
Empiric maintenance dose recommendations differ depending on the age range of the child. For children aged 3 months to less than 12 years, the guidelines recommend 60 to 80mg/kg/day , in divided doses every 6 hours. Recommended dosing for children 12 years and above is 60 to 70mg/kg/day in divided doses given every 6 to 8 hours. Most children should not require more than 3,000 mg/day.
Neonates
Finally, in neonates, the vancomycin dosing guidelines state that a loading dose is not recommended in this population. Doses recommended to achieve an AUC of 400 mg·h/L (assuming a MICBMD of 1 mg/L) in neonates and infants up to 3 months old range from 10mg to 20 mg/kg every 8 to 48 hours, depending on postmenstrual age, weight, and serum creatinine.
Vancomycin Dosing in Special Populations
Vancomycin and Hemodialysis
Other areas addressed in the vancomycin dosing guidelines include dosing of vancomycin in patients receiving various types of dialysis. For patients receiving hemodialysis, a strict weight-based dosing recommendation may provide a useful starting point until serum concentrations have been determined.
Pre-dialysis serum concentration monitoring should be performed at least weekly and drive subsequent dosing.
Pre-dialysis concentrations between 15 and 20mg/L are likely to achieve the AUC of 400 to 600mg.h/L in the previous 24 hours, based on expert opinion in the guidelines.
Specific dosing recommendations are also provided in the vancomycin dosing guidelines for patients receiving hybrid dialysis therapies such as Slow-Low Efficiency Dialysis (SLED) and continuing renal replacement therapy (CRRT).
Finally, another area addressed by the vancomycin dosing guidelines is a continuous infusion. The guidelines provide a discussion on the role of continuous infusion therapies which may provide a reasonable alternative for certain pediatric and adult patients.
The Path Forward

Now that you have an understanding of the vancomycin dosing guidelines and the changes recommended, it is important to move forward with your clinical team in this change management process and prepare for the changes.
DoseMe has supported hundreds of customers with the transition from trough based dosing to AUC-guided vancomycin dosing.
We can offer the following resources to help your team get started:
- Basic Definitions: DoseMe provides a vancomycin pharmacokinetics refresher that is a helpful resource for pharmacy staff and clinicians.
- Education: Enroll in our online and self-paced free CE courses to learn about AUC-based dosing and Bayesian dosing.
- Literature Review: Explore this compilation of independent research related to AUC-based monitoring of vancomycin.
- Bayesian Dosing: Learn how a Bayesian dosing software, such as DoseMeRx, can support your vancomycin monitoring program.
- Vancomycin AUC Conversion Toolkit: Download all of these resources, plus other helpful implementation tips and checklists in a concise document.
If you would like to learn more about how we can support your transition to AUC-based vancomycin dosing, please email me at kkuper@dosemehealth.com or call (832) 358 3308.
I would be happy to share more insights into how we have supported other institutions through this change management process.
Try DoseMeRx For Free
We support vancomycin dosing AUC calculations with a wide range of vancomycin models using DoseMeRx – a bayesian dosing calculator. Try the DoseMeRx free online AUC dosing calculator or evaluate the full DoseMeRx platform free for 14-days. Start trial now →
Related Articles

References
- Rybak M, Le J, Lodise TP, et al. Therapeutic monitoring of vancomycin for serious methicillin-resistant Staphylococcus aureus infections: A revised consensus guideline and review by the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, the Pediatric Infectious Diseases Society, and the Society of Infectious Diseases Pharmacists. Am J Health-Sys Pharm. 2020; (in press).
- Rybak M, Lomaestro B, Rotschafer JC, et al. Therapeutic monitoring of vancomycin in adult patients: a consensus review of the American Society of Health-System Pharmacists, the Infectious Diseases Society of America, and the Society of Infectious Diseases Pharmacists. Am J Health Syst Pharm. 2009 Jan 1;66(1):82-98
- Zonozi R, Wu A, Shin J, et al. Elevated vancomycin trough levels in a tertiary health system: frequency, risk factors, and prognosis. Mayo Clin Proc. 2019;94(1):17-26
- Aljefri DM, Avedissian SN, Rhodes NJ, et al. Vancomycin area under the curve and acute kidney injury: a meta-analysis. Clin Infect Dis. 2019 Nov 13;69(11):1881-1887.
- Sader HS, Farrell DJ, Flamm RK, Jones RN. Activity of ceftaroline and comparator agents tested against Staphylococcus aureus from patients with bloodstream infections in US medical centres (2009-13). J Antimicrob Chemother. 2015; 70(7):2053-2056.
- Pai MP, Neely M, Rodvold KA, Lodise TP. Innovative approaches to optimizing the delivery of vancomycin in individual patients. Adv Drug Deliv Rev. 2014; 77:50-57.
- Rybak MJ, Vidaillac C, Sader HS, et al. Evaluation of vancomycin susceptibility testing for methicillin-resistant Staphylococcus aureus: comparison of Etest and three automated testing methods. J Clin Microbiol 2013;51(7):2077-81.
- Donagher J, Martin JH, Barras MA. Individualised medicine: why we need Bayesian dosing. Intern Med J 2017’47(5):593-0600


